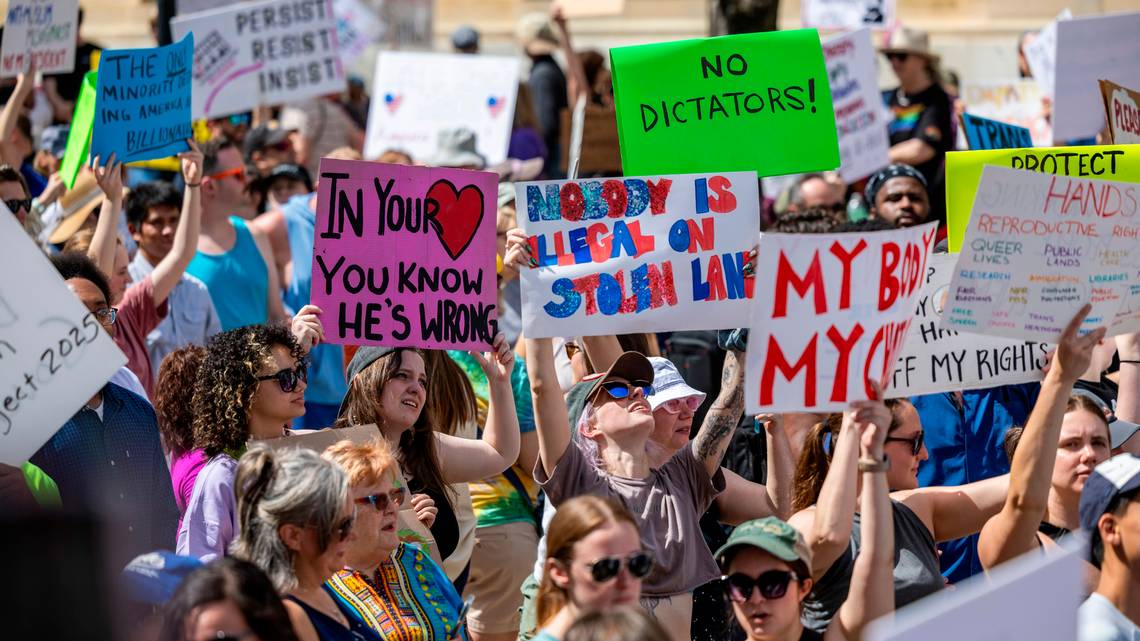How to choose where to live when you are older: age in place or in a long term care facility?
Author: Marianna Crane
After a long career in nursing--I was one of the first certified gerontological nurse practitioners--I am now a writer. My writings center around patients I have had over the years that continue to haunt my memory unless I record their stories. In addition, I write about growing older, confronting ageism, creativity and food.
My memoir, "Stories from the Tenth Floor Clinic: A Nurse Practitioner Remembers" is available where ever books are sold.
Lois, Happy 84th Birthday
Remembering Lois on her 84th birthday.
Learning about Artificial Intelligence
Learning about AI and how to make my blogs better.
It’s Never Too Late For Old Dogs To Break Old Habits
Making life changes in our old age.
The Pull of the Ocean
Changing our mind about a family beach vacation.
My Daughter, the Architect
A Modern House Tour celebrating women architects and my daughter.
The Blessings of a Screened Porch
Listening to the bird songs on a spring day soothes the troubled mind.
A Day at the Hands Off Protest: Unity in Diversity
Five older women attend a protest rally.
I’m No Longer in Charge
Learning late in life when to let go.
How to Survive: Build a Community
Supported by your community, you will be more likelyto make a difference in our current malfunctioning political world.